Wars are won one battle at a time
If you follow the cancer space closely, you will know that flashy headlines around cancer ‘cures’ are invariably irresponsible or at least vastly exaggerated. Genuine therapeutic progress comes about slowly & many of the most promising advances in oncology have stemmed from targeting select tumor types on the basis of antigen expression or other ‘bespoke’ characteristics. Notably, Eli Lilly acquired Loxo Oncology for about $8bn earlier this year, largely due to the promise of Loxo’s small molecule RET inhibitor LOXO-292 (in-licensed from Array Biopharma). RET fusions can lead to uncontrolled cell growth, a hallmark feature of cancer.
LOXO-292 is an outlier both in terms of efficacy and in terms of the diminutively small target population, estimated at a few thousand patients in the United States. Other ‘oncogenes’ have a more broad appeal all the while remaining ‘precision medicines’.
Precision medicine with broad appeal
Inhibition of another mutated protein implicated in cell proliferation, a GTPase known as KRAS, has been on the mind of cancer drug developers for quite some time. KRAS plays an important role in cell proliferation, and mutated forms of the characteristically spherical and smoothly folded protein have been implicated in carcinogenesis.

Given that KRAS mutations are associated with a significant portion of colorectal and lung cancers, and given that expression of these ‘oncogenes’ is also associated with resistance to existing therapies and poor survival outcomes, targeting KRAS mutations is a compelling drug development proposition. However, KRAS has long been considered to be essentially “undruggable” due to the lack of binding sites on the protein.

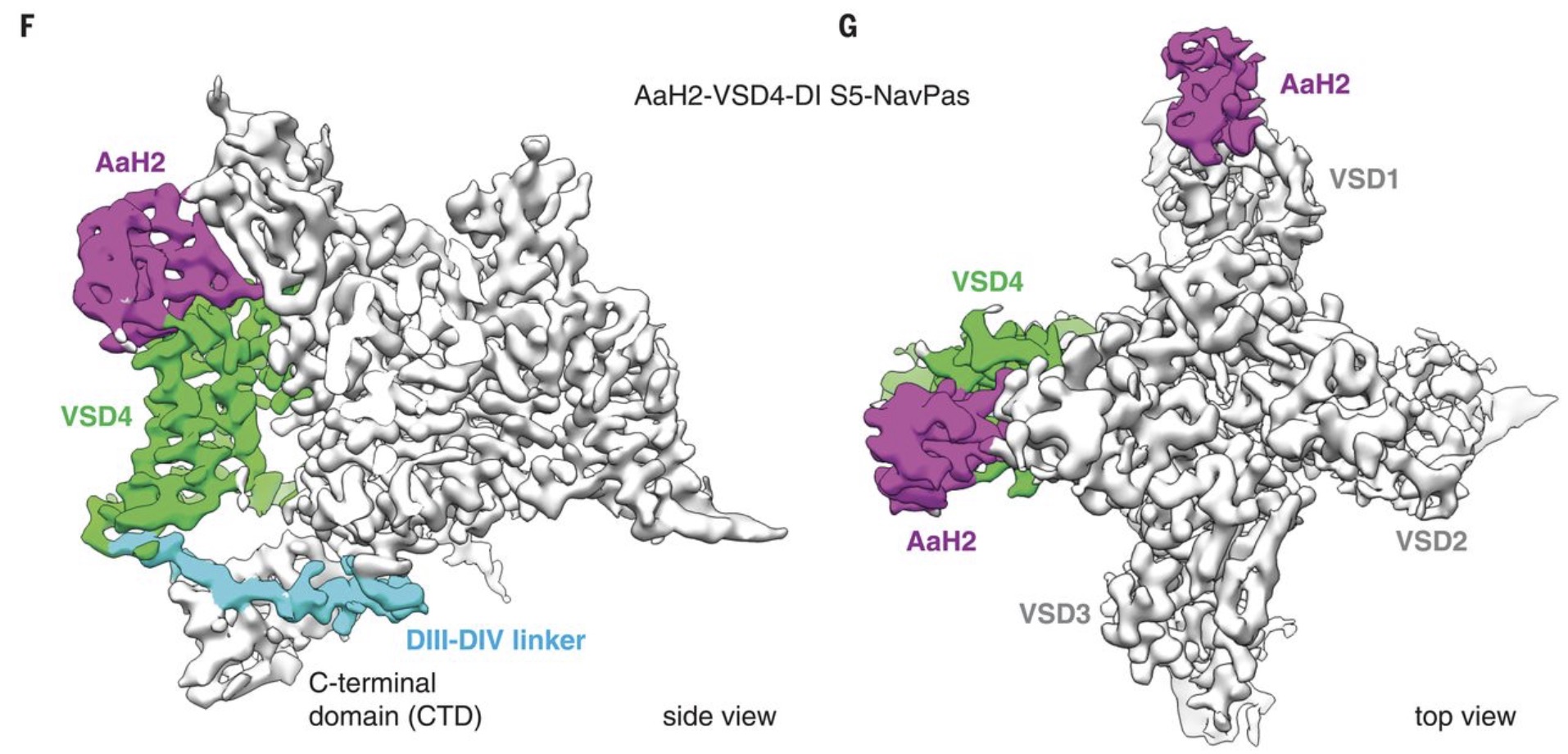
Fortunately, one particular flavor of mutated KRAS known as ‘G12C’ presents with a cysteine en lieu of a glycine, which presents an opportunity for irreversible, covalent binding. In the case of AMG 510, the drug candidate binds to the cysteine (highlighted in yellow in the image above) and induces a conformational change by ‘flipping up’ a histidine residue (in red).
This very elegant example of structural biology & chemical engineering enabled Amgen to go forward with a compound that features an acceptable safety profile and which ticks the boxes of precision medicine & a patient-friendly, oral route of administration.
Preliminary data from PhI pilot trial show AMG 510’s promise
The clinicaltrials.gov entry for Amgen’s PhI trial shows that the company began enrolling patients in August 2018, with a starting dose of 180mg once daily. The goal of a pilot / dose escalation trial such as this is to characterize the drug’s PK/PD, tolerability and to identify initial efficacy signals. The AMG 510 trial is typical in that it enrolls patients who are heavily pre-treated; thus testing the KRAS inhibitor, as monotherapy, in a setting with high unmet medical need. Positive outcomes would demonstrate the drug’s standalone utility all the while strengthening its value proposition as a second- or third-line intervention in otherwise refractory patients.

In time for this year’s ASCO conference, we now have an initial readout from this ongoing trial, with 9 patients evaluable at the time of the data cutoff. Of these 9, 1 showed a partial response, 6 showed stable disease and 2 showed disease progression. Amgen also report that 1 additional patient showed a partial response following the data cutoff. These data drew mixed reactions, which is likely indicative of unrealistic expectations perhaps stoked by the likes of LOXO-292 in RET.
While this sample is simply too small to draw any firm conclusions, it certainly points to AMG 510 being a viable KRAS G12C inhibitor. Preliminary subgroup analysis could also be suggestive of KRAS inhibition predominantly benefiting the NSCLC population. Amgen already announced during their most recent quarterly call that they plan to initiate studies with AMG 510 in combination with immuno-oncology agents such as PD-1/PD-L1 inhibitors, which could potentiate 510’s (likely) “tumor-static” effect with a strengthened immune response. Should 510 continue to show a stronger signal in NSCLC than in colorectal cancer, it seems likely that Amgen would focus on lung cancer which has a poor survival prognosis & as a result, greater unmet need than colorectal.
‘Sympathy moves’ of a competitor could be unjustified
Mirati Therapeutics, a biotech R&D shop, is also advancing a KRAS inhibitor. Although the drug’s chemical structure is unknown and there is no telling whether it will match AMG 510’s performance, Mirati shares have appreciated more than 20-fold over the past 2 years:

Now valued at more than $2bn, MRTX looks very risky ahead of an initial readout from MRTX849. The drug will either be a home-run, beating Amgen at their own game, in which case Mirati would see further appreciation, or it could fall woefully short of expectations and destroy much of MRTX’ value in the blink of an eye.
Given just how tough it is to target KRAS, and seeing how a (presumably) successful KRAS inhibitor like 510 does not lend itself to miracle outcomes, MRTX bulls may very well have gotten ahead of themselves:
A positive readout from MRTX would evidently be good for patients, as more therapeutic options against a promising pathway are never a bad thing. KRAS has certainly piqued my interest following these initial AMG 510 impressions and given the drug’s MOA & tolerability, it seems plausible that promising preclinical findings in combination with immuno-oncology agents could be replicated in-human.